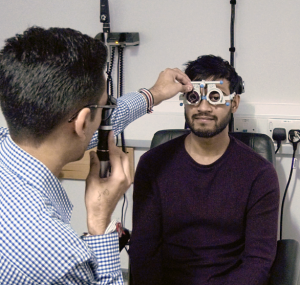
Investigating optometric and orthoptic conditions in autistic adults
Dr Ketan Parmar summarises the findings from his study where he conducted eye examination on autistic adults. The researchers involved in the study were Drs Emma Gowen and Catherine Porter and Professor Chris Dickinson. The academic team collaborated with autistic individuals, Peter Baimbridge and James Pelham. This was part of a series of studies forming Ketan’s PhD. For more information please visit our website.
Rationale and objectives
Sensory issues are common amongst autistic people. As a result, they can experience difficulties with bright environments, lights, patterns, colours and movements. Also, autistic children are more likely to require spectacles, have eye coordination problems (e.g., a turned eye) and develop a lazy eye. Based on this it can be assumed that autistic people will visit an optometrist regularly. Unfortunately, autistic people can face difficulties accessing healthcare, and have poor experiences of healthcare services.
Research up until now has focused on autistic children, many of whom also had a learning disability. We set out to investigate visual conditions in autistic adults without learning disabilities, who are currently underrepresented. We provided eye examinations for autistic adults to gain an understanding of presenting eye conditions in this group. We also conducted interviews with the participants to get more detailed information on the accessibility of eye examinations.
What happened during the study
Participants underwent a thorough eye examination which checked spectacle prescription, eye coordination and sensitivity to patterns (visual stress). At specific points during the eye examination, participants were asked questions about which eye tests they didn’t like and why, which tests they liked and how the experience could be improved.
Upon completion, participants were dispensed new spectacles or eye exercises if required. They attended follow-up appointments to review these.
Additionally, at the beginning and end of this study, we asked participants to complete three questionnaires. These measured: autistic visual sensory experiences, how vision affected daily tasks, and the quality of vision when doing close work. We investigated whether providing new spectacles or treating eye coordination problems affected the outcomes of these questionnaires.
Who took part?
A total of 24 autistic adults without learning disabilities attended for an eye examination; 14 identified as male, 9 as female and 1 as non-binary.
The age range of the participants was 18-67 years. The majority of participants wore spectacles and had undergone an eye examination within the last 2 years. Some participants also wore tinted lenses.
What we found
Participants presented with a wide range of optometric (spectacle related) and orthoptic (eye coordination related) issues, although they may not have necessarily been experiencing symptoms for these:
- 20 participants needed their spectacle prescription updating
- 15 participants had an eye coordination anomaly
- 6 participants had visual stress
Across the study, 19 participants (79.2%) needed new spectacles, and 8 (33.4%) required eye exercises. 1 participant was given tinted lenses. In total, 14 participants (58%) were successfully treated for their presenting eye conditions; the remaining participants were referred for continuing care, didn’t complete the study or withdrew.
Our findings suggest that autistic people are more likely to require frequent spectacle prescription updates than non-autistic people. Additionally, eye coordination and visual stress issues were more common in our participants compared to non-autistic people. Visual stress is usually managed with tinted lenses. We found that providing up-to-date spectacles or treating eye coordination problems reduced the need for tinted lenses.
There were no significant changes in the questionnaire results between the first and second time that participants completed. However, this may be due to the small number of participants taking part in this study, so more research is required to understand the effect of treatment on visual sensory issues.
This study provided useful information on how to make eye examinations more autism-friendly. Autistic people can experience sensory issues during eye examinations due to bright lights or instruments which make physical contact, to name a few. Tests requiring instruments or the optometrist being close felt intrusive and uncomfortable. Our participants appreciated an explanation and clear instructions before each test, and the opportunity to ask questions. They valued not feeling rushed during the examination and having optional breaks, as a result feeling relaxed and comfortable. Participants were sent an information document before the eye examination to help them prepare for the visit. The pictures, descriptions and videos of the different tests were useful to reduce their anxiety. To improve the eye examination, participants recommended rearranging the order of tests so that the more demanding ones are conducted earlier. Also, limiting bursts of background noise would be helpful to prevent distraction.
Future directions
Due to the COVID-19 pandemic, the number of people who could take part in this study was limited. Some of our conclusions need further evidence. We have suggested this study to be repeated on a larger scale.
We have developed guidelines for eyecare providers on how they can provide more autism-friendly services. These give recommendations related to the whole of an eye examination, from the point of booking the appointment through to dispensing any treatment. These guidelines have been published in an international journal.
We have produced resources for autistic patients to help them prepare for eye examinations. These include text descriptions together with images and videos of the various steps involved in an eye examination. These can be found on our website (link below).
We will be giving talks, writing articles for other journals and creating training programmes for eyecare providers to disseminate our findings further.
Further information and the above patient practitioner resources can be found here






0 Comments