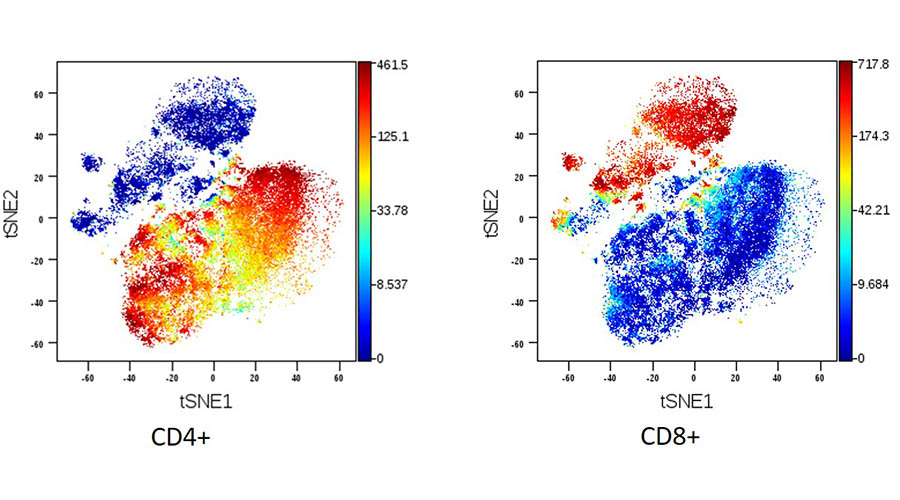
Key insights into the genetics of PsA that explain fundamental differences between psoriasis and PsA.
What was already known?
Psoriatic arthritis (PsA) is an inflammatory condition causing pain and stiffness in joints and tendons. Approximately one third of patients with psoriasis will go on to develop PsA resulting in a reduction in their quality of life caused by increasing disability and additional health complications.
A key area of research within the Arthritis Research UK Centre for Genetics and Genomics in the Centre for Musculoskeletal Research is the identification of risk factors for the development of PsA; this will allow us to understand the underlying cause of disease and ultimately help identify psoriasis patients at high risk of PsA, allowing early treatment to be introduced to reduce the impact of PsA.
What we found?
Our recently published study focuses on the identification of genetic risk factors for PsA; we compared the frequency of genetic variants, referred to as single nucleotide polymorphisms (SNPs), between large numbers of DNA samples from patients with PsA and healthy control samples. When the frequency of the SNP is significantly different between cases and controls, the SNP is said to be associated with risk of developing PsA and this association is interpreted as being important in the disease process.
When we analysed the data from the study we found a new association to SNPs on chromosome 5, and when we investigated these SNPs for association with skin-only psoriasis, we did not find any evidence for association. In addition, we also found SNPs that were specifically associated with PsA at a gene on chromosome 1. This gene is known to be associated with psoriasis, but our results show that there are different SNPs associated with PsA and psoriasis at this gene. Hence, our results identify new SNPs that are specifically associated with PsA.
What is the benefit to the public?
Identifying which cells are the key drivers of inflammation in PsA will help us to focus on how the genetic changes act in those cells to cause disease. Our results show that many of the PsA associated SNPs occur in regions of the genome that are important in the function of CD8+ cells, an important cell type in the immune system, and identify this as the key cell type to focus on in future studies.
In conclusion, our recent study begins to reveal key insights into the genetics of PsA that begin to explain fundamental differences between psoriasis and PsA.
Publications
(Bowes J, et al. Nature Communications (2015) 6, 6046. eScholarID:258775 | PMID:25651891 | DOI:10.1038/ncomms7046)

0 Comments