Outcome measures for systemic sclerosis-related Raynaud’s phenomenon
What was already known?
Raynaud’s phenomenon (RP, periodic colour changes of the fingers, usually in response to cold exposure) is associated with poor blood flow and is one of the key problems for patients with scleroderma (a rare disease, also known as systemic sclerosis). Raynaud’s phenomenon causes pain, numbness and loss of hand function. In patients with scleroderma it can progress to open wounds (ulcers) on the fingers that can become infected or gangrenous requiring surgery. The impact of impaired hand function is felt not only on activities of everyday living, but also on childcare and employment.
Clinical trials to investigate new treatments have been hampered by the lack of ‘outcome measures’ (the way that we assess whether a treatment is having an effect on the disease process) by which to measure any benefit. Existing outcome measures, for example asking patients to keep a record of the number of Raynaud’s attacks, are subjective and not always sensitive to change. At the moment there is no validated (proven) objective measure of changes in blood flow or skin temperature in the hands of patients with scleroderma.
The aim of this study was to validate two non-invasive imaging techniques in patients with scleroderma and RP through the collaboration of six UK specialist scleroderma centres. One imaging technique measured blood flow (laser speckle imaging), and the other measured skin temperature (thermography). Thermography assessment included both ‘standard’ (i.e. hospital-based) thermography and low-cost mobile-device based thermography. Low-cost devices may be useful for measurements at clinic visits, or even at the GPs or at home in the future.
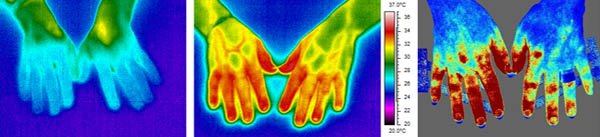
Figure: (Left) False colour thermal image of hands post cooling and (middle) after 15 minutes rewarming showing skin temperature. Temperature scale shown on the on the right hand side of the thermal images; cooler skin appears blue; warmer, green/yellow; (right) laser speckle imaging showing blood flow in hands after 15 minutes (red represents higher blood flow, blue relatively lower)
What was discovered?
Six specialist scleroderma centres (Manchester, Bath, Cambridge, Leeds, London and Newcastle) recruited 159 patients with scleroderma-related RP who attended on two consecutive days. During each visit, following acclimatisation to room temperature, the patients placed their rubber-gloved hands into cold water (15oC) for one minute. Immediately before immersing their hands, and for 15 minutes after removing their hands from water and gloves, the patients’ skin blood flow and temperature were simultaneously recorded to examine how the blood flow and temperature returned to pre-immersion levels. Measurements were made from these images to assess:
- Reliability (repeatability); day-to-day agreement and agreement between observers who read the images.
- Validity; how the change in measurements using the different imaging techniques, during the course of the cold challenge, compared to each other.
This is the first multi-centre study examining reliability and validity of cold challenge in patients with scleroderma-related RP using these techniques. Measures of blood flow and skin temperature were found to have substantial reliability and very high validity.
Why is this study important? What is the benefit to patients?
This study proves that both techniques are suitable objective measurement techniques for multicentre clinical trials of new treatments. This finding will facilitate new clinical trials which will help evaluate new treatments which may be more effective than existing ones. These methods may be applicable to clinical trials of all groups of patients with RP, including primary RP, which is very common. Therefore many people stand to benefit.
Publications
(Wilkinson JD. et al. (2018). A multicentre study of validity and reliability of responses to hand cold challenge as measured by laser speckle contrast imaging and thermography: outcome measures for systemic sclerosis-related Raynaud’s phenomenon. Arthritis Rheumatol 2018;70 (6): 903-911. PMID:29457381| DOI:10.1002/art.40457)

0 Comments