Student Perspective on Disaster Mental Health
In the light of a world experiencing more and more disasters as the years go on, I want to talk about a little-focussed area of study: disaster mental health. This topic holds a special place in my heart as I, myself, have struggled with mental health issues my entire life, and that’s without the added stress of a disaster! It has pushed me to become an advocate for mental health, and I wish to shine a much-needed light on its importance, not simply in everyday life, but after a traumatic event. The inevitability of disasters fascinates me, and thus when it came to considering what field I wish to go into, disaster mental health gave me a platform where I believe my humanitarian efforts and values will be best fitted.
In this blog, in addition to giving a brief introduction on disaster mental health, I want to encourage others to consider its importance and explore the role mental (in)stability plays in recovery from disaster. This blog highlights the multi-dimensionality of disaster mental health, busting the myth that disasters ultimately leave people in a perpetual state of mental distress. Although people do tend to be worse off post-disaster, in many cases it is possible to recover.
What is it disaster mental health?
Disaster mental health is an emerging area of research, with most studies focussing on visible outcomes of disasters, for example, the loss of tangible items (homes, livelihoods, businesses, etc.) and the subsequent economic and development impacts. However, such losses also have a profound effect on mental health. The persistence of mental distress can only be rectified if dedicated action is taken because, as unfortunate as it is, mental health issues linger.
Material reality, after a period of time, returns to a form of normality, but many people’s mental health may function at a different pace, with feelings of dread, insecurity and distressing thoughts becoming all encompassing. “Traumatic events are not easy for anyone to comprehend”, nor should someone who has experienced such an event be expected to bounce back instantly (Morganstein, 2019: 1). The development of psychiatric disorders, such as post-traumatic stress (PTSD) and anxiety, present themselves after disaster; they represent one’s true feelings, no matter the façade they may present. So, if this is case, why isn’t disaster mental health more focussed upon?
Why is disaster mental health important?
Disasters are an “inevitable aspect of life” due to the confluence of natural hazards and societal decisions (Schulenberg, 2016: 1223). Thus, it is imperative to consider all disaster impacts, including mental health. Further, the climate crisis is exacerbating disaster frequency and intensity (Gruebner et al., 2017). Such hazardous events, leave communities at risk of low mood, depression, anxiety, and even PTSD. Of course, mental distress can occur at any point throughout someone’s life, whenever a traumatic experience overwhelms personal coping abilities (CDCP, 2018). This is a trigger point for a breakdown in mental stability.
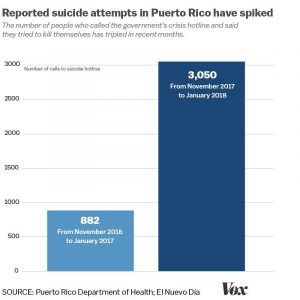
However, increased exposure to traumatic social and environmental disasters invites mental distress into communities. Many are left in a state of poor mental health for years after experiencing a disaster, and it is only with help from others that they can resume a sense of normality. For example, in the weeks following Hurricane Maria (2017) suicide attempts in Puerto Rico tripled (Campbell, 2018, and one-fifth of Puerto Ricans reported a need for mental health services (Ferreira, 2021). Therefore, it is important to measure and reflect on mental health regularly pre- and post-disaster, to lessen long-term issues.
Multi-dimensionality of post-disaster mental health
Disaster mental health is a multi-dimensional area of research. It extends beyond negative impacts and emotions, exploring stories of people positively transformed by disaster. Many individuals come out of disastrous situations better than before. They use the event to build back better and experience a new, more profound meaning to life (Riffle et al., 2020). This mental status is labelled: post-traumatic growth.
Post-traumatic growth is the best possible outcome after a disaster. Bouncing back quickly from adversity is difficult, but with collaborative support it is achievable. It all depends on how the person processes events, their social conditions prior to a disaster, and their general mental stability. Social capital, community linkages, and appreciation of this support contribute to positive growth after a traumatic event. However, “association between social capital[1] and disaster mental health is limited and ambiguous” (Wind et al., 2011: 1).
There has been an increased call for post-disaster mental health resources and support, to create adaptive coping strategies amongst communities. For more communities to experience post-traumatic growth, there needs to be better approaches that provide those affected with the means to progress. There are tools for mental resilience-building that are proven to mediate and mitigate the effects of sudden distress. Even small, seemingly meaningless attempts to directly manage stressors, through recognition and processing, can lead to an overall improved state of mind, before, during, and after disaster (Riffle et al., 2020).
Community resilience: what impact does community support have on mental health?
It is established that little attention is given to disaster mental health,but what is worse is that even less attention is paid to the effects of group involvement on mental health, at both community and individual levels (Gallagher et al., 2019). Mental stability, especially in times of crises, relies on community connectedness and social support (Wind et al., 2011). Empirical findings suggest that “social support and other psychosocial resources play a key role in reducing the impact of disaster exposure, buffering individuals from various post disaster stressors” (Gallagher et al., 2019: 167). Community shapes mental health impacts (Kawachi et al., 2008),

Diagram to highlight the direct link between the community and mental care. Source: Prewitt et al., 2006, Advances in Disaster Mental Health and Psychological Support.
To help someone post-disaster, mental aid work does not necessarily need to be clinical. You simply need to be a friendly neighbour and offer support, even just listening goes a long way. Support does not always mean you need to be diagnosed or seek medical help, sometimes people just need a friend, and I think, particularly post-disaster, to maintain a steady level of mental stability, having a friend, a community base, forms the foundations to keep on moving forward.
Looking Forward
Disaster mental health is complex. Everybody responds and reacts differently, however, this shouldn’t discourage researchers. Mental health is just as important, arguably more important, than physical health and must be taken into more consideration in future disaster responses. It is important to educate communities about disaster mental health, so that they too can reap the benefits of being more resilient characters in the future (Schulenberg, 2016; Ferreira, 2021).
References
Asian Disaster Reduction Centre (ADRC), 2019. Information on disaster risk reduction of the member countries: Philippines. Available at: https://www.adrc.asia/nationinformation.php?NationCode=608
Campbell, A., 2018. ‘Calls to Puerto Rico’s suicide hotline have skyrocketed since Hurricane Maria’. Available at: https://www.vox.com/policy-and-politics/2018/2/21/17032168/puerto-rico-suicide-hotline-hurricane-maria
Centre for Disease Control and Prevention (CDCP), 2018. Learn about Mental Health. Available at: https://www.cdc.gov/mentalhealth/learn/index.htm
Climate-Adapt, 2016. Hyogo Framework for Action 2005-2015: Building the resilience of nations and communities to disaster. Available at: https://climate-adapt.eea.europa.eu/metadata/publications/hyogo-framework-for-action-2005-2015-building-the-resilience-of-nations-and-communities-to-disasters
Ferreira, R., 2021. The Road to Mental Health Recovery after Disaster. Tulane University. Available at: https://socialwork.tulane.edu/blog/disaster-mental-health
Gallagher, H., C., Block, K., Gibbs, L., Forbes, D., Lusher, D., Molyneaux, R., Richardson, J., Pattinson, P., MacDougall, C., and Bryant, R., A., 2019. The Effect of Group Involvement on Post-disaster Mental Health: A Longitudinal Multilevel Analysis. Pgs., 167-175.
Gruebner, O., Lowe, S., R., Sykora, M., Shankardass, K., Subramanian, V., and Galea, S., 2017. A Novel Surveillance Approach for Disaster Mental Health.
Kawachi, I., Subramanian, S.V. and Kim, D., 2008. Social capital and health. Pgs., 1-26.
Morganstein, J., C., 2019. Coping after Disaster. Available at: https://psychiatry.org/patients-families/coping-after-disaster-trauma
Morganstein, J., C., and Ursano, R., J., 2020. Ecological Disaster and Mental Health: Causes, Consequences, and Interventions.
Poteyeva, M., 2018. Social Capital. Encyclopaedia Britannica. Available at: https://www.britannica.com/topic/social-capital
Prewitt, J., O., Lakshminarayana, R., and Murthy, S., 2006. Advances in Disaster Mental Health and Psychological Support.
Riffle, O., M., Lewis, P., R., and Tedeschi, R., G., 2020. Posttraumatic Growth after disasters, in Positive Psychological Approaches to Disaster. Pgs., 155-167.
Schulenberg, S., E., 2016. Disaster Mental Health and Positive Psychology – Considering Context and Natural and Technological Disaster: An Introduction to the Special Issue. Pgs., 1223-1233.
Wind, T., R., Fordsham, M., and Komproe, I., H., 2011. Social Capital and Post-disaster Mental Health.
[1] Definition: a concept that revolves around relationships between people and their interconnectedness within society (Poteyeva, 2018).



0 Comments